
If you’ve ever wondered… Can gluten affect your skin?
Absolutely.
Your skin is the largest organ of your body and plays a key role in protecting your body from harm against toxins, bacteria, viruses, UV light and general trauma.
It’s also one of the many windows to potential inner turmoil in your body that’s brewing beneath the surface.
As you know, there’s an entire industry built around helping you obtain luxurious skin from the outside. But what you might not realize is that no amount of creams and potions that can mask issues like long-term dehydration, an unhealthy diet, excessive alcohol consumption, or chronic poor sleep.
Nor can they hide inflammation brought on by gluten, other food sensitivities and allergies and autoimmunity.
Most doctors will tell you that they don’t fully understand what triggers chronic (and often embarrassing) skin issues.
Diet isn’t often on their radar as a hidden root cause underlying various rashes, blisters, bumps and scaly skin that some of us know all too well.
And so the go-to options most dermatologists recommend include medicated creams, ointments and pills might help in the short-term.
But long-term relief often takes a level of desperate dedication of trial and error on your part (or with the help of a practitioner who looks at your condition from a holistic perspective).
To be honest, it’s utterly perplexing that food and diet aren’t considered first in the conversation about skin disorders.
Often people suffer for years without getting straight answers that can result in expensive and ineffective treatments that don’t ultimately work. They’ve got to tick off all the boxes first that frankly are more extreme before going back to the drawing board to wonder if it was diet related the entire time.
It’s worth asking the question… why not opt to examine the low-hanging fruit with diet rather than take something that can long-term negatively impact your health?
For those of us currently living with gluten sensitivity, celiac disease, and other autoimmune disorders, food is often a big piece of every health puzzle that’s encountered. And that’s why those of us that struggled for years without clear diagnoses know all too well the pain and frustration involved with finding the root cause of ongoing skin issues.
Can Gluten Affect Your Skin?
 The simple answer is yes.
The simple answer is yes.
It’s been known for quite some time that reactions to gluten can absolutely manifest as skin issues.
Why dermatologists aren’t quite up to speed with this is unfortunate for the patients in their care.
On one hand, it might not be their fault — a simple search of the American Academy of Dermatology’s website looking for any mention of gluten turns up absolutely nothing.
Surprisingly, dermatitis herpetiformis that’s clearly been linked to Celiac Disease and thus the ingestion of gluten, is not listed anywhere on their site.
(This is still true as of 2/20/2017 — it is not listed their Diseases and Treatments section. Kind of a big omission, right?)
Think about when you saw a dermatologist with an unresolvable rash. Were you ever asked about your diet?
Unless the doctor thinks that a food is a potential allergen, what you eat is rarely a subject for conversation.
The Downside To Treating Your Skin Only On The Outside
Instead, exterior salves are prescribed that may or may not resolve the problem.
Every single one of them has their own set of side effects, some more horrible than others. Make sure you know the long-term issues before starting on them and understand why they often don’t work.
 Aside from the fact that uncomfortable skin disorders can make everyday life physically irritating flares of eczema, psoriasis, dermatitis herpetiformis or other autoimmune skin conditions can be emotionally and mentally draining as well.
Aside from the fact that uncomfortable skin disorders can make everyday life physically irritating flares of eczema, psoriasis, dermatitis herpetiformis or other autoimmune skin conditions can be emotionally and mentally draining as well.
For example, if you suffer from cycles of psoriasis outbreaks, you may feel embarrassed and very self-conscious of rashes, lesions or scabs.
The shame can make you feel that your only option is to cover up the exposed skin.
This means going to different lengths to conceal the blemishes by wearing long sleeves in the summer. Or avoiding bathing suits altogether.
It can make you avoid prolonged contact with other people for fear of being teased or stared at.
For children with skin issues, bullying is a serious concern as other kids don’t always take too kindly to even the smallest of differences.
While other things such as environmental allergies, personal care products, and metals (such as nickel) can certainly cause issues with skin flare-ups, you should consider the potential control you have over your skin through diet. Gluten skin problems are more common than you might think which makes diet a better (more effective option).
And diet changes are less expensive and involve fewer side effects than drugs on the market used to manage autoimmune skin conditions such as Humira.
Gluten Skin Problem #1 — Psoriasis
Psoriasis is the most prevalent autoimmune disease in the United States as well as one of the most readily visible affecting 7.5 million people in the U.S. alone.
It’s characterized by a few different symptoms that include:
– red patches of skin (sometimes covered with a silvery scaly texture)
– dry or cracked skin
– small or larger scaling areas
– scabbing
– bleeding
 This said, why not consider gluten as a culprit when organizations like the National Psoriasis Foundation states that up to 25% of people who have psoriasis also may be sensitive to gluten.
This said, why not consider gluten as a culprit when organizations like the National Psoriasis Foundation states that up to 25% of people who have psoriasis also may be sensitive to gluten.
And that’s taking into account the people with psoriasis who have a gluten skin problem that they know about.
Additionally, the Journal of Clinical Laboratory Analysis found that psoriasis patients with the HLA CW6 gene (that’s linked to psoriasis) had an increased sensitivity to the gliadin protein (gluten).
Of those patients, approximately 16% of patients had either IgA and/or IgG antibodies to the protein. When these patients tried a gluten-free diet, the majority found a marked improvement in their symptoms.
(Oh… and this study was done in 2000 which again underscores the question of why gluten isn’t typically suspected by dermatologists.)
Another form of psoriasis is psoriatic arthritis which is characterized by inflammation, swelling, and pain of the joints throughout the body along with classic psoriasis symptoms.
It too has also be linked to gluten sensitivity.
In 2002, a study was published in the Journal of Rheumatology found that 49 of 302 patients with psoriatic arthritis had increased serum IgA antibodies to gliadin (gluten protein). When 30 of these 49 patients followed a gluten‐free diet, their psoriasis improved.
Gluten Skin Problem #2 — Eczema
Like psoriasis, millions of people suffer from eczema, an itchy, inflamed, and irritated skin condition. Sometimes it’s called general dermatitis that can strike any part of the body.
To be fair, eczema is not always caused by food sensitivities. But many sufferers have found that eliminating offending foods such as gluten and dairy can make a real difference.
The National Eczema Association (NEA) agrees, and has posted the following statement on their web page under alternative therapies for eczema:
“There is no doubt, however, that some foods seem to be inflammatory, particularly in some people, and so gluten-free and dairy-free may make a difference in some. Avoiding processed foods is also generally a good idea, even if it does not help the eczema much. Eating natural, organic, and balanced foods is a win-win, so rather than argue against it, it is better to encourage it!”
To be clear, a gluten-free diet or dairy-free diet may not work for everyone. However, it’s a risk worth taking (in my opinion) if nothing else seems to work.
Alternatively, the University of Maryland Medical Center lists food allergies as a significant factor for some eczema sufferers.
They suggest that eating a healthful diet and avoiding common food allergens may reduce inflammation and symptoms. Some of the main food culprits include:
- dairy (HERE’S how I swap dairy out of client’s diets)
- wheat (sometimes all gluten-containing grains — HERE’S a comprehensive list)
- soy
- citrus
- peanuts
- fish
- eggs
- corn
- tomatoes
One study even suggests an emphasis on gluten and dairy specifically as culprits of eczema. The researchers found that antigen absorption (of gluten and dairy) from the gut can play a role in the beginning stages of atopic eczema.
A great, real-life example of food sensitivity and food allergy elimination to help treat eczema can be found at the phenomenal blog, Itchy Little World, written by a mother of two detailing her family’s ups, downs, and ultimately successes controlling her son’s severe allergies and eczema.
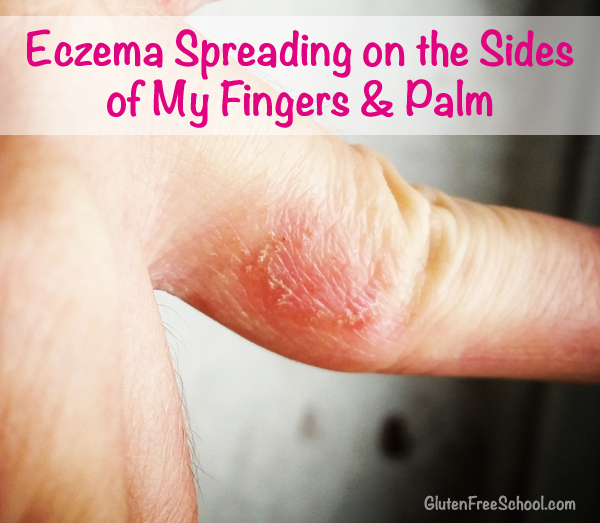 Even Jennifer, the founder of Skinterrupt, has talked about the embarrassing nightmare of developing dyshidrotic eczema.
Even Jennifer, the founder of Skinterrupt, has talked about the embarrassing nightmare of developing dyshidrotic eczema.
She always had strange clear bumps on the side of her right middle finger, but suddenly they became red, inflamed, terribly itchy and would burn if exposed to pretty much anything including water.
Even washing her hands went from being a painful chore to near impossible. Soap and water would only exacerbate the issue.
She shared her experience on THIS podcast!
You can see a picture here of one of Jennifer’s flares.
After doing a lot of internet research, she narrowed down her condition and then went to a dermatologist who didn’t have any answers for her.
“Basically the dermatologist assumed that I must be using all sorts of harsh, chemically lotions and soap or wearing nickel (as that can sometimes cause skin flares). None of that was true.
“Aside from her suggestion that it was stress related, the doctor said that the reason people develop dyshidrotic eczema really isn’t clear. She wasn’t concerned about my diet and refused to speak about it.”
Aside from prescribing a steroid cream (which can permanently thin your skin), “she suggested that I keep the affected areas, which were spreading and flaring up with increasing intensity, covered with Vasoline,” shares Jennifer.
Really?
Why is a petroleum-based product a legit recommendation for skin issues?
Through this, Jennifer became very aware of how frustrating skin ailments are.
[Check out our Definitive Guide to Eczema Treatment & 7 Naturally Remedies That Actually Work]
She acknowledges that “I still don’t have concrete answers, but I’ve often wondered why eczema isn’t considered an autoimmune condition or at least related to autoimmunity. If you gain some relief using steroid creams, then we’re missing something because corticosteroids are used to reduce inflammation and suppress your immune system.”
That said, the concept of “leaky skin” should be on your radar since that is a big piece of the puzzle!
Gluten Skin Problem #3 — Dermatitis Herpetiformis (DH)
Dermatitis herpetiformis, simply abbreviated as DH, is a painful rash usually seen in 15-25% of people with Celiac Disease.
Contrary to the name, DH is not caused by the herpes virus.
It is actually a skin manifestation of Celiac. It should be noted that this skin condition is exclusively seen in patients with diagnosed or undiagnosed Celiac Disease.
That’s not to say that those who experience DH can’t also experience psoriasis, eczema, or other skin conditions. They certainly can. Simply put by the National Foundation for Celiac Awareness, a positive diagnosis of DH always indicates a positive test for Celiac.
Interestingly though, those with DH and Celiac may not experience any gastrointestinal discomfort or symptoms.
In many cases of DH, an intestinal biopsy for Celiac can come back negative, since the skin is, in fact, manifesting the symptoms.
Left unchecked, Celiac can lead to the development of other diseases and even cancer. Going gluten-free typically clears up DH symptoms and reduces antibodies to gluten in the body.
Other Notable Skin Disorders
Here are a few other gluten skin problems to be aware of:
- Acne
- Alopecia areata (patchy baldness)
- Prurigo nodularis
- Hyperpigmentation (Vitiligo)
- Several atopic rashes (allergy related)
Here’s a great further listing of associated skin conditions (evidence shows some of these can be present in non-celiac gluten sensitivity as well).
What are your next steps?
If you’ve got chronic skin issues and suspect that gluten is an issue…
OR you’ve been struggling with your chronic skin rash issues for way too long…
It’s time to look at your skin rashes from a fresh perspective that dives deep into the underlying triggers and hidden causes that keep you stuck in the flare cycle.
I’ll be honest… often gluten is just one small piece of the puzzle and there are other non-diet factors that must be addressed.
Granted, it can feel overwhelming especially if you’ve already spent a lot of time without success trying to figure things out on your own. That’s why if you’re committed to getting to the bottom of the issue, it’s time to ask for help.
You don’t have to continue to suffer alone.
I know because I’ve been there. (Read more about my story here.)
And I work with women (and men) who are fed up spinning their wheels without getting any results from their dermatologists who just want to try the same old thing, again and again, hoping for a different result.
If you’re ready to start getting answers that are deeper than just the skin so you can finally resolve the rashes for good, let’s talk!
Pin this Post and Save it for Later








Jennifer, this is a great article ~ thank you for compiling so much detail! I’m an Esthetician and a Holistic Health Coach myself, and in the treatment room, I always bring up diet and ‘undiagnosed food sensitivities’ as a culprit for various skin conditions. Acne and Rosacea are common symptoms of that are diet related, so the mention of Probiotics to start healing their gut is a must. I share your frustration about Dermatologists not getting onboard. But you know, a lot of my clients are looking toward more holistic treatments and I have sought out a more natural treatment plan. HOLISTIC DERMATOLOGY through Acupuncture and Chinese herbs can make all the difference ~ so something to keep in mind 🙂 I had a condition where my eyes and eyelids would itch like crazy, and then go through this cycle of being swollen, inflamed, then dry and get crusty. It was so frustrating because this flare up would occur intermittently. I changed my eye makeup, I went to an eye doctor, and I tried eye drops…with no results. After a 28 day cleanse, and going back to my ‘go-to’ foods, flour products included…I had the most aggressive flare up of hives – on my face, my eyes and my neck. It finally started to dawn on me that something I was eating was the culprit. After reading Wheat Belly, and seeking the advice of an acupuncturist who advised me to get off gluten & dairy, did I ultimately wake up to the realization and had to ’emotionally’ face this head on and change my ways. Denial is a HUGE part of this game we play with ourselves 🙁 I had not made the connection to wheat (and possibly gluten) for almost 4 YEARS! So, you’re right, Celiac symptoms are not always the clue…there are so many other symptoms to consider. I am seeking the treatment from an Integrative doc, here in Philly to get actual test results, but doing your own investigating can move the process along.
What about acne? Can gluten contribute to acne for some people?
One of the symptoms of my wheat allergy is acne—tiny pimples on my cheeks, shoulders and upper arms, and sometimes stomach. For me, this is the clearest symptom when I consume any amount of wheat, as I don’t have significant digestive issues. Though not as serious as celiac, my sensitivity is enough for me to avoid eating any wheat.
I have dh and refused to take the recommended dapzone. I went as gluten free as possible without being fanatical. I was still having breakouts and then I read an article that said to take l glutemine and dietary enzymes that contain ipss in them. Ever since I started this regimen I have not had another outbreak. Yay!!! Just wanted to share with others who might be looking for an answer.
I have had a hand eczema for 5 years or so. It came on after some stress. I went gluten, dairy, corn and soy free this past September and now it’s all over my calves too. It’s itchy and horrible looking. I changed my diet as I also have some environmental/chemical sensitivities. I just got tested for leaky gut and thyroid. Results will be out in a couple of weeks. Skin stuff is very frustrating.
I was diagnosed with Granuloma Annulare over 30 years I have taken steroids, had steroid shots injected into my “spots”. Nothing seemed to clear it up. While it is not contagious, it looks like I had bruising all over my arms and legs I was very self conscious. My dermatologist never discussed food issues with me. Until my daughter was in school to become a dietitian, and was dealing with Celiac and other food sensitivities herself, did the GA become clear. She has her own practice in functional medicine and worked with me for testing food sensitivities and what she found was that I had a severe gluten sensitivity as well as other sensitivities and since I have illuminated and other food triggers my GA has gone away. Hooray! I can’t stress enough to others that some of their skin issues may be a result of gluten in their daily intake. So I thank my daughter for insisting I get tested. A return on our investment! I feel and look great!
I have been tested & recieved confirmation that I have gluten & soy allergies. I struggle with eating the right foods. I went gluten & soy free 4 2yrs. It make me lose weight & feel great. I’m now going on 2yrs of bad diet & I have rashes all the time & I’ve swollen up like a balloon. It’s a vicious cycle of depression, lack of goals & lack of determination to be on the right track. I’m working on a new me and this information makes me feel better about myself. I’m going to be a better/more difficult person to eat with but it will make me love myself more
Hey Megan, know that you’re certainly not alone. And even I understand how personally challenging a change in diet can be no matter how much good it will do. I’m glad that this information can be an inspiration to you and know that getting support to get you over the hump so that you do get (and STAY) on the wagon may be a worthwhile endeavor to consider. There are many out there who can do that for you, including myself if you’re serious and know that a helping hand will get you there faster than continuing to struggle on your own.
Sincerely,
Jennifer
I’ve been suffering what seems to be dh for over a year. I have had numerous blood tests, biopsies and skin scrapings, all looking for this or that, but everything coming up negative. I keep telling my doctors that I think it’s systematic, some type of allergy. while they were treating me for things like scabies, I took myself of of my anti anxiety meds and my bipolar meds. nothing was working. after much research on line I am convinced I have dh. I’m trying to get my doctors to test me but I couldn’t wait and have gone gluten free. now I see that may give a false negative. I’m trying to get a prescription for dapsone, but a false negative won’t get me the script. my entire body is covered, head to toe. I am in extreme pain and not sleeping.
Christie, it’s my understanding that to be tested for DH, they do a skin biopsy. If you still have the rash, they can still biopsy it. You can have DH and have inconclusive results from celiac testing… so don’t fret. Get your rash biopsied. See more info here: http://celiac.nih.gov/Dermatitis.aspx
Thank you for sharing that article. Skin issues have plagued me (and my family) for ever. I have very dry skin. The “cure” is slather on all these petroleum based grease products, until you clothes cling to your skin.
We also get thin skin as we age, with my siblings and I we can see our father’s skin developing on each of us.
Itching is also an issue. Yesterday, working outside but not touching plants, I developed an allegoric reaction rash, itchy and painful, that went away quickly with cortisone cream (which I use only in extreme circumstances).
I am completely gluten free, mostly dairy free and very careful about which vegetables I eat, as some will cause more problems. I have not found a good lotion that works, though some are much better than others.. (please no scents).
What I did do was try detergents and laundry soaps until I found one that doesn’t cause me to itch. I also took all sulfate related products out of my body care routine, causing problems in how to wash my hair.
Skin…. sigh…
I had a horrible rash several years ago on shoulders and arms. Now I have scars in those areas and lumps of scar tissue in spots where I pick at the skin. I’m what is known as a picker and have picker’s nodules per the dermatologist. Still struggling with picking. I’t another manifestation of OCD; had many different incarnations of it. This is only the latest but the most obvious. Would like a solution and how to heal the scars. Also, sometimes get itchy spots which I scratch and sometimes tear the skin. The spots are some type of flare, get very hot and itchy for no apparent reason. Sometimes also get hot tender spots, especially on the palms of hands. No idea what these are but I believe they are an arthritic manifestation.
After 15 years of suffering with incredibly itchy red patches roaming from my head to my feet, I read an article that gluten allergies can cause itchy skin. My dermatologist and I had tried removing scent, dyes, and utilizing steroids but the itch never went away. Once i read the article, I removed gluten from my diet. Within a week, my skin was perfectly clear. I truly can’t believe I suffered for so long, just not knowing. I have now gone months without a single itchy episode…..I cannot tell you what a relief it is.
What about Melasma? Can a sensitivity to gluten cause that?
I have had a facial rash only for 3 yrs, getting worse, itchy, red, inflammed (not little bumps) just awful patches all over face, I was patch tested, offending culprits eliminated, food sensitivity, nothing noted, blood work for numerous things negative except slightly higher eosinophil which doctors say due to fighting allergy, steroid creams do nothing except thin my skin. A round of prednisone helps but when stopped comes back. I’m miserable, feel ugly as heck, embarrassed, mortified and depressed. I am in a people business and am simply ready to give up. Could gluten be the culprit? I stopped eating all wheat about a week ago, no difference yet. I have nowhere to turn except complete isolation…
i was diagnosed by 2 dermatologists to have perioral dermatitis. nothing they prescribed helped. I kept a food diary and found if I went GF the rash immediately cleared up. just a small amount of gluten will make the rash break out again. I hope this will help others with this problem. Marie